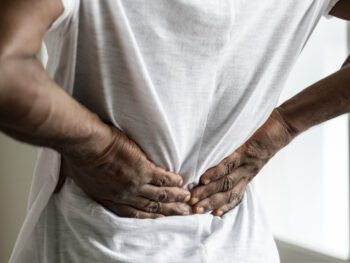
Chronic pain can not only impact the quality of your life but also lead to additional health issues if left untreated. …
Understanding Compounding Strategies for Pain ManagementRead More

Chronic pain can not only impact the quality of your life but also lead to additional health issues if left untreated. …
Understanding Compounding Strategies for Pain ManagementRead More

The AXIS Pharmacy Northwest has selected Laura Gifford, Pharmacist for its Employee Spotlight! Rich Molitor, R.Ph., …
AXIS Pharmacy Northwest Employee Spotlight – Pharmacist Laura GiffordRead More

Sofie has been with AXIS since she was 16 years old when she began working as a Pharmacy Assistant in the pharmacy's …
AXIS Pharmacy Northwest Names Sofiya Zhydovlenko Employee of the Quarter for Q4 2021Read More

Compounded preparations are medications that are tailor-made for you from your provider’s specifications. They are …
Why Choose AXIS? – 5 Reasons Why We Are Your Preferred Compounding PharmacyRead More

This holiday season, AXIS Pharmacy Northwest is proud to support CASA (Court Appointed Special Advocate) for Children by …
AXIS Teams with CASA to Bring Joy to Foster Children This Holiday SeasonRead More

AXIS Pharmacy Northwest has awarded Dee Dee Carpenter, compounding technician, the honor of "Employee of the Quarter" …
AXIS Pharmacy Northwest Names Dee Dee Carpenter “Employee of the Quarter” for Q3 2021Read More
AXIS Pharmacy has named Certified Pharmacy Technician Gurmit Kaur, Employee of the Quarter for Q2 2021. Rich Molitor, …

AXIS Pharmacy Northwest is proud to announce that we now have the Moderna 19 COVID Vaccine available! Call us today …
Moderna 19 COVID Vaccine Now Available at AXIS Pharmacy NorthwestRead More

AXIS Pharmacy Northwest has named Fred Gomez, Compounding Pharmacy Technician, the Employee of the Quarter for 1st …
AXIS Pharmacy Northwest Names Fred Gomez “Employee of the Quarter” for 1st Quarter, 2021Read More
The Snohomish County Coronavirus Response & Community Resource Hub provides a wealth of information and the latest …
On-Site COVID-19 Vaccinations for Adult Family Homes in Snohomish CountyRead More

AXIS Pharmacy Northwest is proud to announce that Dr. Victoria Wang of VCA Crown Hill Animal Hospital in Seattle, …

Nataliia Glotov is a pharmacy technician who has been with AXIS for three years. When asked why she was selected …
24255 Van Ry Blvd, Suite A2
Mountlake Terrace, WA 98043
Main Line: 425.672.5800
Compounding: 425.672.5820
Long Term Care: 425.672.5810
